30 years later, Minn. doctor still opening doors in fight against AIDS
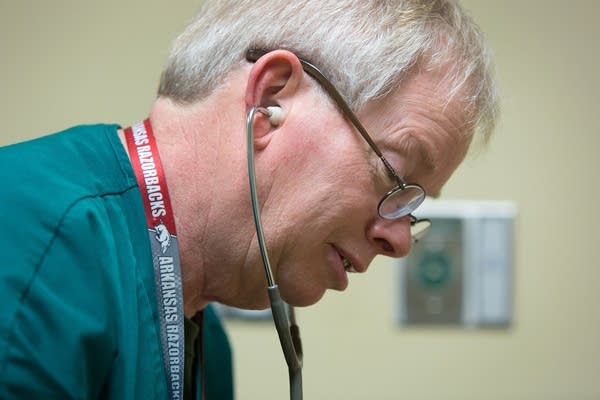
Dr. Keith Henry examines a patient at the Positive Care Center at Hennepin County Medical Center in Minneapolis, where he treats patients living with HIV.
Jennifer Simonson / MPR News
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.



