Hope for brain cancer treatment after canine success
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.
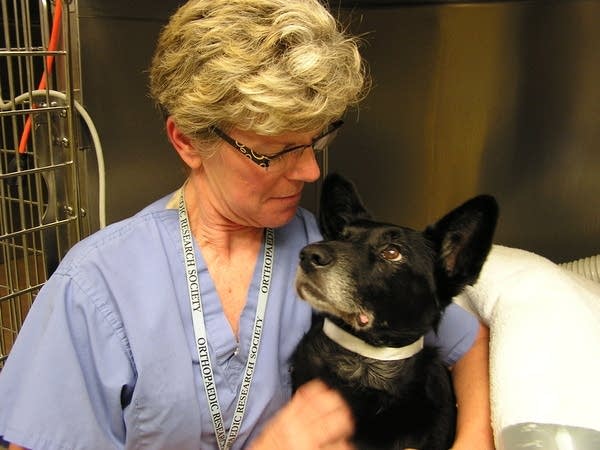
One year ago, researchers at the University of Minnesota began an experimental procedure to save a dog from an aggressive brain tumor.
By treating Batman, a mixed-breed German shepherd, the University of Minnesota's College of Veterinary Medicine researchers hoped to gain valuable insights into new ways of treating brain tumors in humans.
Veterinary surgeon G. Elizabeth Pluhar has spent the past year caring for Batman during his cancer treatment. After months of good progress reports, Wednesday was his final visit her lab for a brain scan.
Pluhar had already looked at some images that showed no signs of cancer, but the true measure of success was a series of contrast photos that were still loading into the computer Wednesday.
Turn Up Your Support
MPR News helps you turn down the noise and build shared understanding. Turn up your support for this public resource and keep trusted journalism accessible to all.
"It's a little difficult (to see) because there's scar tissue in there, too," Pluhar says.
Scar tissue from Batman's surgery looks a little suspicious when you see it on his scan, but a trained eye like Pluhar's knows it's nothing to worry about. A few moments later, she gives the all clear.
"I don't see any tumor right now," she says. "Which is wonderful."
Batman's recovery is remarkable. The 13-year-old shepard mix had a very aggressive form of brain cancer called a glioma. It's the same type of cancer Massachusetts Sen. Ted Kennedy is battling.
Gliomas are tricky to treat because they send out little tentacles that infiltrate other parts of the brain, and surgery alone usually isn't sufficient to cure a glioma.

So university researchers from the vet school, the medical school and the Masonic Cancer Center devised a treatment for Batman that began with surgery. After that, the dog received gene therapy and a custom-made, anti-cancer vaccine designed to boost his immune system.
Researcher John Ohlfest, who helped create the new immune therapies, said the vaccine is made up of dead cancer cells from Batman's tumor that have been enhanced in a way that makes them much more obvious to the dog's immune system.
Ohlfest can't say exactly why the vaccine has worked so well, but his team is working feverishly to figure it out.
"We've gone through, well, Hypothesis A, Hypothesis B, Hypothesis C, why is it better?" he said. "I think we're on Hypothesis S by now, but we're getting very close. We're very close to understanding it."
That answer will be very important in determining whether the treatment could be used on people some day, and it's not by chance that researchers are trying out their experimental cancer treatments on dogs.
Ohlfest said dogs are actually a much better animal model for testing brain cancer treatments because they're big enough to operate on and they're also big enough to handle treatment doses that would be comparable to what a human might need. Those factors have been major stumbling blocks in applying rodent studies to humans.
"The problem is that over 90 percent of cancer therapies that have worked in mice have failed in people," Ohlfest said. "Not only did they fail, but toxicities that were not observed in mice occurred in people, so it's double-edged bad news there."
So far, the university's experiment has been nothing but good news for Batman.
Pluhar says her patient appears to be in perfect health.
"Being a year out and still having no sign of any tumor, no evidence of disease, is amazing," she said. "Because I do think that had we done nothing or had we just done surgery that he would not be alive right now."
Pluhar and Ohlfest have secured funding to treat another 60 to 70 dogs with brain cancer as part of their clinical trial, and they've enrolled about a half dozen so far.
All of the treatments are free for participating in the research. Normally the treatments would cost up to $20,000 for people without pet insurance.




