Minnesota researchers on the cusp of a diabetes cure
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.

The cure for diabetes could come from cells from pigs being raised in germ-free pens in Western Wisconsin or from human skin cells in a lab on the University of Minnesota campus.
Those two experiments are part of a joint project launched one year ago by the University of Minnesota and the Mayo Clinic to defeat diabetes within the next 10 years. The effort is called the Decade of Discovery.
It's high-stakes research. Diabetes is a worldwide epidemic that is taking a huge toll in Minnesota. Health officials say one-third of all adults in Minnesota either have diabetes or are pre-diabetic, with blood glucose levels that are higher than normal.
ISLET CELLS FROM PIGS
Turn Up Your Support
MPR News helps you turn down the noise and build shared understanding. Turn up your support for this public resource and keep trusted journalism accessible to all.
With genetic characteristics that are remarkably similar to humans, pigs may hold the cure to diabetes. There is such promise in the animals that a nonprofit organization built a facility in western Wisconsin to supply pigs, or more specifically their insulin-producing cells, to University of Minnesota transplant researchers.
Insulin is a crucial hormone that helps us use energy from the food we eat. People with diabetes have lost their insulin cells or they don't work properly.

The pigs at the Spring Point Project -- placed in special pens where they are isolated from human germs -- could one day provide an unlimited supply of pancreatic, insulin-producing cells to all diabetic patients who need them.
"They are special because they are raised in this barrier facility, essentially in a bubble separated from the outside world," said Tom Spizzo, the project's executive director. "We can make sure that their health is extremely high so that we're minimizing the risk of transmission of any agents from the donated materials into the recipients."
In the more than four decades since the U of M performed the world's first pancreas transplant, only a few thousand severely ill diabetic patients have received donor organs or the clusters of insulin-producing cells that are called islets. There simply aren't enough donor pancreases to go around.
Nobody knows if pancreatic islet cells from pigs will effectively produce insulin in humans. The Food and Drug Administration has not yet given the university permission to proceed with human clinical trials. But U of M transplant surgeon Bernhard Hering said transplanted pig islets have worked in other animals he's tested.
"We have been able to show that we can reverse diabetes in monkeys for many, many months, for close to a year," Hering said. "Many people could not believe this and thought that is completely impossible."
At the earliest, the injecting of pig islet cells in humans could begin within a year. But it would likely take many more years to obtain FDA approval to market a new treatment.
ISLETS DEVELOPED FROM OTHER TYPES OF CELLS
Researchers at the U of M are working on other promising treatments as well.
Stem cell researcher Meri Firpo is studying whether human skin cells can be transformed into insulin-producing cells to treat diabetes. Her technique erases the cell's original purpose before giving it a new assignment.

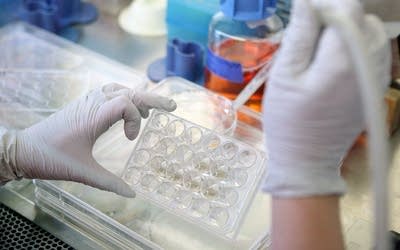
"Right now all the cells in this plate are unspecified," Firpo said. "So they've been completely reprogrammed from the purpose they had as a skin cell into a cell that could become literally any cell type in the body."
The new cells Firpo creates closely resemble pancreatic islet cells. When she puts them into laboratory animals the cells secrete insulin. Firpo can't reveal much more about her research until it has been reviewed and published. But she said her discovery is also a big step forward in diabetes research.
"It seemed so improbable or even impossible," she said. "But we actually are making the progress that we expected to. And we fully intend to do what we say we will do. We will cure diabetes."
Like Dr. Hering, Firpo also has to prove first that her cells could be used safely in humans.
ARTIFICIAL PANCREAS
While Decade of Discovery scientists search for a cure for diabetes, other researchers are focused on perfecting the devices diabetics already use to manage their disease.
One technology that could be available soon is an artificial pancreas that more precisely regulates blood sugar. It's also referred to as a closed-loop system.

Current methods of measuring blood sugar are not very precise, since glucose monitor readings are about 20 minutes old by the time a patient sees them and programs that information into their insulin pump. By using an artificial pancreas that receives information from an activity monitor which measures how many calories a person burns, researchers aim to make such devices communicate more precisely with each other.
Research groups around the world have been experimenting with "closing the loop" between insulin pumps and glucose monitors used by diabetics. Researchers think they can do so in much the same way pacemakers regulate hearts.
Dr. Yogish Kudva, a Mayo Clinic endocrinologist, described a prototype of an artificial pancreas as a "continuous glucose sensor and transmitter."
A couple of the devices in his laboratory are as small as a pager. The computer that links them together is about the size of a smartphone.
"Our studies are essentially to make the software better and to individualize the software for each patient," Kudva said.
To study the effectiveness of the devices, Mayo researchers are trying to figure out how many calories a person really burns in a day, because activity determines the amount of insulin a person needs. In order for an artificial pancreas to deliver insulin as perfectly as the human body, the device needs to be programmed accurately to account for even the tiniest of movements.
In one test, 32-year-old diabetic Melissa Mulder, of Plainview, Minn., took part in an experiment that measured her activity over a period of five days.

"Twenty minutes where I sat, 20 minutes where I walked on the treadmill, 20 minutes where I sat, just back and forth, back and forth," Mulder said. "It was the most structured study that I'd ever done."
Mulder, who has had diabetes for 17 years, said she gets very upset with herself when her blood sugar levels fluctuate because she knows she's damaging her body. She thinks a machine could do a better job.
"I wouldn't have to worry about those long-term complications so much, keeping my numbers so tight, trying to do it on my own," she said. "We always hear about the long-term complications of diabetes. And it's inevitable, no matter how well of a job that I'm doing."
The system could revolutionize diabetes care, said Dr. James Levine, a member of the team working on Mayo's artificial pancreas. But it's not a cure.
"I don't think any of us believe that these machine-based solutions and equations will ever be perfect," Levine said. "What we're trying to do is to close the gap between substantial imperfection and a better solution for real patients living in the real world."
Mayo has yet to test its artificial pancreas system on patients. But researchers in Europe have tested a similar system on two diabetics.
Researchers in France and Italy each connected a patient to the devices for 24 hours while a team of doctors and computer engineers monitored their health. The patients, who each ate a meal at a restaurant and then spent a night in a hotel where they were monitored by research teams, were able to attain near-normal glucose levels for one night.
That marked a significant advance because, for the first time, patients were able to control their diabetes using an artificial pancreas in a real-life setting.
Kudva hopes that within two years he will be able to test Mayo's artificial pancreas on the first human patients in the United States.