Data: Nearly 1 billion pain pills flooded Minnesota during height of opioid crisis
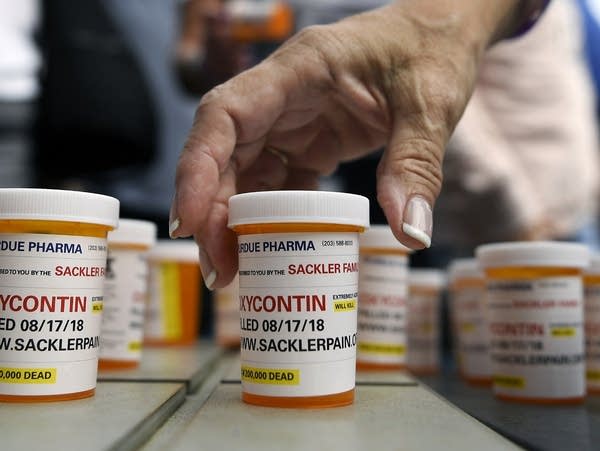
Family and friends who have lost loved ones to OxyContin and opioid overdoses leave pill bottles in protest outside the headquarters of Purdue Pharma in Stamford, Conn., in August 2018. Data made available by the Washington Post show a link between prescribing practices and rising opioid overdose deaths in Minnesota and across the country.
Jessica Hill | AP
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.



