Vaccines, public health and personal choice
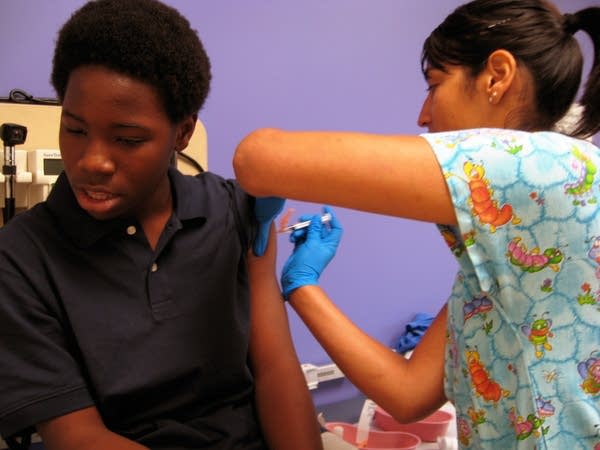
Vashaud Jones, 12, grimaces as nurse Marieli Guzman injects him with his measles, mumps and rubella booster shot on Thursday, Aug. 31, 2011 at Children's Hospitals and Clinics of Minnesota in Minneapolis.
Lorna Benson | MPR News 2011
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.



