Some COVID-19 tests come with a bill. Here’s how to avoid one
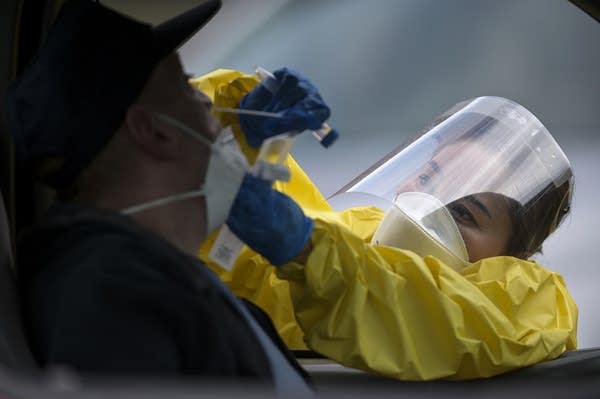
Elizabeth Santoro, a medic with the Minnesota Air National Guard 133rd Medical Group, administers a free COVID-19 test to Thomas Harmon at the Minneapolis Armory on May 23.
Aaron Lavinsky | Star Tribune via AP file
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.



