As Minn. rolls through first round of vaccinations, some providers worry about being left out
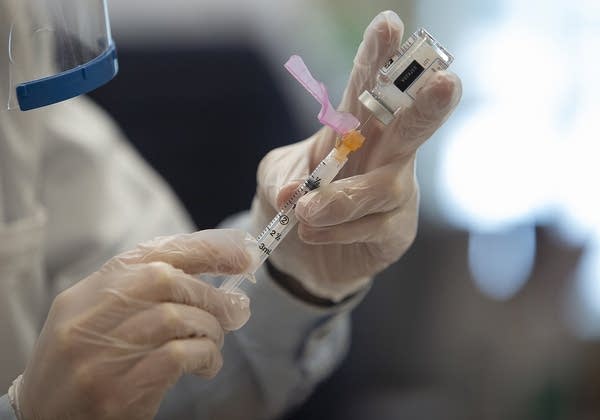
Pharmacist Dan Cook prepares a dose of the COVID-19 vaccine at the Gardens of Episcopal Homes in St. Paul. Residents and employees in the long-term care facility began getting vaccinated on Dec. 30, 2020.
Christine T. Nguyen | MPR News 2020
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.



