One Minn. health care provider using AI to prioritize patients for COVID-19 shots
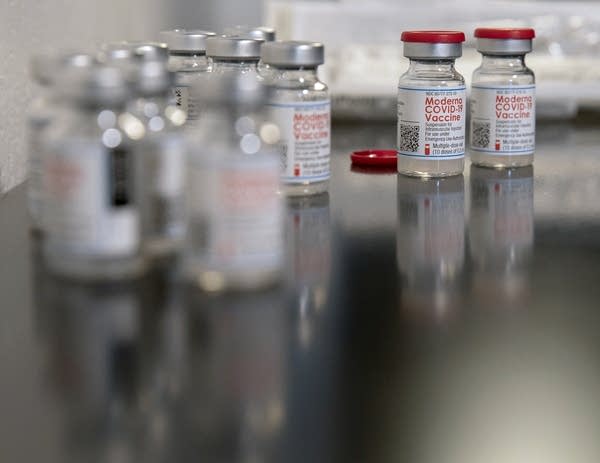
Vials of Moderna COVID-19 vaccines sit on a table at United Family Medicine in St. Paul in January. The state Health Department has mostly left decisions around prioritizing vaccine distribution within eligible groups up to individual health care providers. Many are prioritizing their patients based on age, but others are taking a more complicated approach.
Christine T. Nguyen | MPR News file
Go Deeper.
Create an account or log in to save stories.
Like this?
Thanks for liking this story! We have added it to a list of your favorite stories.



